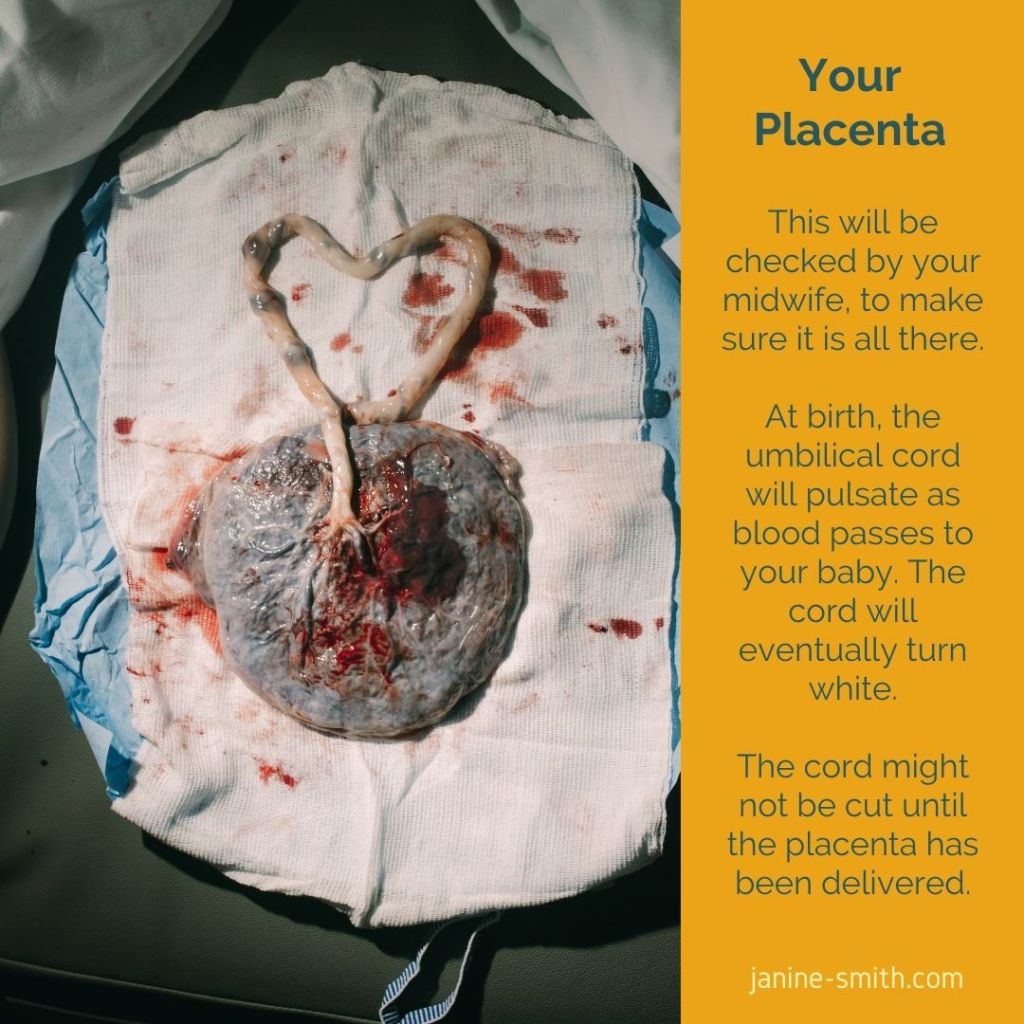
After your baby has been born, your placenta needs to follow shortly afterwards. You can relax as you cuddle your baby but your midwife will stay focused on you until your placenta has been safely delivered.
You may have some options with how this is managed.
Natural/Physiological Method
- If you have had a straightforward birth without drugs you can choose to deliver your placenta without drugs.
- The umbilical cord remains untouched and you can cuddle and feed your baby, which produces oxytocin to create contractions and aid the delivery of your placenta.
- It can take between 10-60 minutes to deliver your placenta and your contractions will be noticeable but probably quite mild compared to labour.
Managed/Active Method
- If you need or choose drugs to manage the delivery of your placenta, you will be given an injection of Syntocinon/ Syntometrine to create contractions. The umbilical cord will then be clamped and cut. You can continue to cuddle and feed your baby throughout.
- Once the placenta has separated from your uterus, you may need to push but your midwife will also help by using controlled cord traction – gently pulling on the cord. It can take between 10-30 minutes to deliver your placenta and your contractions may be noticeable but mild compared to labour.
Delayed Cord Clamping
- It is now recommended to delay the clamping of the umbilical cord so that babies can benefit from having more of the oxygenated blood from the placenta – this provides 30% more blood and increased iron levels for your baby for up to 6 months.
- Babies already benefit from this with the natural method of placenta delivery but, in many births, there can now be a delay of up to 5 minutes before having the injection in the managed method. This also includes with a Caesarean and with pre-mature babies.
- This may not be an option if there are any problems with your placenta or umbilical cord or of there are any concerns about your baby.
Potential Complications
Prolonged 3rd stage: if the delivery of your placenta takes longer than 60 minutes (natural) or 30 minutes (managed) your midwife will assess you and drugs may be needed to manage and speed up the delivery of your placenta.
Retained Placenta: this happens when the uterus stops contracting or when the placenta remains attached to the wall of the uterus. If the drugs don’t help with the delivery of the placenta, it will need to be manually removed by an obstetrician.
This involves going into the operating theatre, having a spinal or an epidural so you are awake but unable to feel anything apart from some pressure. You will be on an operating table, your legs will be in stirrups and your doctor will use her hand to remove your placenta.
You will be given antibiotics as well as more drugs to help your uterus contract and shrink down.
Sometimes the placenta is delivered but a small piece is retained and you may become aware of this at home – you may experience heavy bleeding, painful tummy cramps, a fever, a smelly discharge and feeling unwell. Contact your midwife or maternity unit because this will need to be investigated and treated.
Retained placenta happens in 3% of births.
Haemorrhage: a minor primary post-partum haemorrhage is a bleed of between 500-1000ml. Drugs will be given to stop the bleed. Most women are well enough to be able to cope with this blood loss. This happens in 5 in 100 births.
A major primary post-partum haemorrhage is a bleed over 1000ml, which is rare but serious. This will require drugs to stop the bleeding and a blood transfusion may also be needed in severe cases. This happens in 6 in 1000 births.
A primary post-partum haemorrhage takes place in the 24 hours after birth can be caused by retained placenta, a low lying placenta, a multiple pregnancy, polyhydramnios, a high BMI, induction, caesarean or a fast labour.
A secondary post-partum haemorrhage of over 500ml can happen between 24 hours and 12 weeks after birth and can involve passing a large clot – bigger than a 50p – or a gush of blood.
Tell your midwife and call the maternity unit so this can be investigated and treated. A secondary post-partum haemorrhage can happen after a primary post-partum haemorrhage and retained placenta. This happens in 2 out of 100 births.
Your care during the third stage
After your baby has been born, your midwife will be assessing you for any bleeding and to observe your general condition and well-being.
If the delivery of your placenta is taking longer than your midwife would like she may suggest emptying your bladder and changing position. If she feels this hasn’t helped or if there is any bleeding, she will probably need to use drugs to manage the delivery of your placenta.
If the delivery of your placenta does become more complicated, your midwife should keep you informed of what is going to happen. But make sure you also ask any questions to feel more informed and reassured.
Welcome To Your Antenatal Course
1. Labour
2. Birth
3. Pain Management
4. Labour & Birth Challenges
5. Meeting Your Baby
6. Your New Baby
7. Relax & Breathe Resources
And please don’t hesitate to message me below to arrange a conversation with me to talk through your questions.

Leave a Reply